Types of urinary incontinence
There are various types of incontinence that lead to urinary leaks, each with unique challenges.
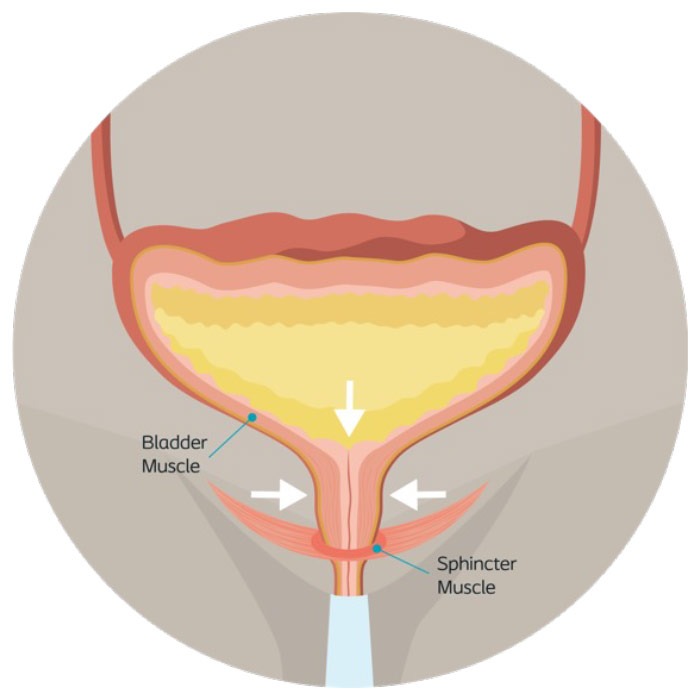
How does the bladder work?
Before we jump into how a bladder can begin to leak, let’s discover how it functions properly.
Urinary function starts with your brain and spinal cord, which work together to direct the urinary system.
When your urinary system is functioning normally, you can control when to hold and release urine. When your bladder becomes full, it sends a signal to your brain, which in turn sends a message to the bladder to release urine into the urethra. The urethral sphincter muscle, which surrounds the urethra, opens and closes the bladder neck – it will contract to temporarily hold urine, or release itself to allow urine to leave your body through the urethra.
3 types of urine leakage
Women often show symptoms or more than one type of urine leakage, so it is important to seek a specialist to ensure you receive the correct diagnosis and find the treatment that is right for you.
Stress urinary incontinence1
Stress urinary incontinence, also known as SUI, is a type of bladder leakage where urine leaks out of the bladder when stress or pressure is applied to the bladder when you run, jump, cough, sneeze, laugh, etc. The urine leaks out even if you do not feel the urge to go to the bathroom. It can be a small amount or a large amount depending on the severity of the incontinence.1
The word “stress” does not relate to the emotional toll associated with the condition, rather to the physical strain associated with leakage.
SUI occurs more frequently among women, especially those who have given birth.
Learn more about the causes and the symptoms of stress urinary incontinence.
Overactive bladder / Urge urinary incontinence1
Overactive bladder (OAB), also known as Urge Urinary Incontinence (UUI), occurs when you feel a strong, urgent need to urinate that you can’t ignore. With OAB, your brain tells your bladder to empty too often even when it isn’t full, or the bladder muscles become too active. This causes the urge (need) to urinate. This “gotta go” feeling makes you fear you will leak if you don’t get to a bathroom right away. OAB can also result in having to urinate many times during the day and/or night.
OAB affects more than 40% of women and 30% of men in the U.S. OAB is more likely in women after menopause. OAB can get in the way of your work, social life, exercise and sleep. However, there are a number of treatments options that can help. They include life style changes, drugs that relax the bladder muscle, or surgery.
Mixed incontinence1
This condition is a combination of both SUI and OAB, where the individual experiences both stress and urge symptoms, which can be challenging to navigate in day-to-day life.

Are you experiencing similar symptoms? Not sure if you have SUI?
To help you better understand your symptoms and take the first step toward relief, we invite you to fill out this quick, free, and confidential self-assessment.
Help is on the way.
